- Home
- About ANT
-
Products
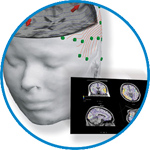
asa
asa is a highly flexible EEG/ERP and MEG analysis package with a variety of source reconstruction, signal analysis and MRI processing features.
.jpg)
eego mylab
The new frontier in multimodal brain research. With up to 16 kHz sampling rate, 256 EEG channels and unique software features, eego mylab gives you an unprecedented in-depth understanding of the human brain.

eego sports
eego sports offers complete freedom to collect high-density EEG data, bipolar EMG signals, and a variety of physiological sensor data, wherever and whenever required, with publish quality data in less than 15 minutes!

waveguard net
The waveguard net sets a new standard for research applications requiring high-density EEG data acquisition with quick preparation time, high flexibility, and subject comfort.
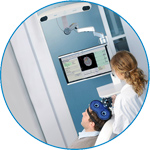
visor2
Our new and upgraded visor2 solutions integrate all the latest technologies for navigated rTMS, dual-coil navigation support, EEG-TMS recordings and pre-surgical evaluation for the highest quality in research and clinical procedures.
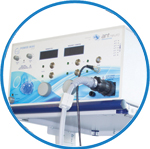
powerMAG ANT
The PowerMAG ANT 100 rTMS stimulator is designed for the specific needs of high-end TMS applications. Powerful high-frequency TMS as well as high precise single pulse and repetitive pulse protocols are combined in one single device.

xensor
xensor offers the solution for digitization of 3D electrode positions. xensor takes care of the whole procedure; it records, visualizes and stores positions acquired with a dedicated digitizer.

waveguard original
waveguard original is the cap solution for EEG measurements compatible with fMRI, MEG and TMS system. Use of active shielding guarantees performance in even the most demanding environments.
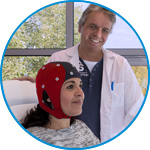
waveguard connect
waveguard connect EEG caps are a perfect match for hospitals and institutes aiming at reliable EEG, maximum uptime and great patient comfort! For optimal signal quality, the electrodes are made of pure, solid tin.

waveguard touch
waveguard touch is a dry electrode EEG cap. The unique Ag/AgCl coated soft polymer electrodes provide stable, research-grade EEG signals while maintaining subject comfort. The combination of these innovative dry electrodes and the industry-leading waveguard cap makes waveguard touch the best solution for dry EEG.
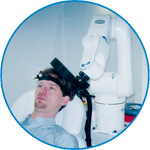
smartmove
smartmove allows planning of a complete TMS session ahead by defining stimulation sites based on anatomical MRI information and functional information like fMRI, PET or EEG/MEG.
Stay - References
- Support
- Events
- News
- Contact Us
You are here
Focal seizure induced by preoperative navigated transcranial magnetic stimulation in a patient with anaplastic oligoastrocytoma
Focal seizure induced by preoperative navigated transcranial magnetic stimulation in a patient with anaplastic oligoastrocytoma
We report the following TMS-related seizure. The subject was a 41 year old woman with the diagnosis of an anaplastic oligoastrocytoma (WHO grade III) located at the right sensorimotor region. The patient underwent subtotal tumor resection 4 years ago with adjuvant chemotherapy and radiation. Due to a progression of the tumor with slight arm paresis, another surgical resection was planned. The patient had the following risk factors for TMSinduced seizure: brain tumor, prior brain surgery, occasional (every 6e8 weeks) symptomatic focal seizures with transient Todd Paresis for a couple of hours. Anticonvulsive treatment with levetirazetam 500 mg b. i. d. was discontinued by the patient earlier due to agitation and mood change. Thus, her medication only consisted of sertraline 100 mg q. d. On the day of the event, the subject had no additional risk factors.
1. Setup
The patient underwent MRI based navigated TMS for motor cortex mapping, which was performed as clinical routine procedure before brain surgery [1]. TMS pulses were delivered through a Magstim 200 (The Magstim Co. Ltd., Whitland, UK) connected to a figure of eight shaped coil using monophasic pulses with anteriorposterior directed currents. A successive mapping of both motor cortices with stepwise increasing stimulation intensity of the first dorsal interosseous muscle was performed during EMG controlled active contraction in order to keep the stimulation intensity as low as possible. Single TMS pulses were repeatedly applied every 5 sec ± 10%. Two sessions of the right hemisphere and one session for the left hemisphere were performed alternatingly. In total about 120e130 single pulses were applied divided in three sessions.
2. Procedure
The patient was sitting in a comfortable reclining examination chair in the TMS laboratory of our outpatient clinic. The investigators were two experienced neurologists and one postdoctoral fellow. After defining the vertex, TMS was started 5 cm lateral and 1 cm anterior to the vertex. First mapping of the right hemisphere was initiated by moving the stimulation location in steps of 0,5 to 1 cm with increasing intensity up to 80% maximal stimulator output (MSO) to locate the primary motor cortex electrophysiologically. A total of about 100 pulses were applied, but no MEPs could reproducibly be elicited probably due to the tumor affecting either the motor cortex or the pyramidal tract. In the second session TMS over the left hemisphere with about 20 pulses were applied in order to locate left M1, which succeeded easily. Then again TMS of the right hemisphere was initiated, this time based on MRI navigation starting at the lateral border of the tumor and MR morphologically suspected hand area. Within 5 pulses a focal motor seizure occurred, starting with myoclonic jerks in the left hand which then gradually spread to the left shoulder. The seizure selfterminated within 3e4 minutes and the application of anticonvulsive medicationwas not necessary. The patient remained conscious throughout the whole seizure episode. After seizure termination muscle weakness was increased by means of Todd paresis which the patient confirmed to be returned to baseline within a day. An EEG or laboratory examination was not done. A follow up brain MRI, which was performed in the following week for surgical planning, revealed no newaspects apart from the known progression of the tumor. There were no additional seizures during the following week until she underwent surgical resection of the tumor again. The clinical diagnosis of this event was TMS-related focal motor seizure due to its typical presentation, which was also familiar to the patient.
3. Discussion
There are several possible mechanisms of action leading to this seizure episode in our case. First single pulse TMS could have directly activated the stimulated area. There are few reports on single pulse TMS inducing a seizure especially in patients with neurological disorders, but also in healthy subjects [2e6]. It is possible that in our patient with potentially increased cortical excitability single pulse TMSwas strong enough to induce a seizure. The second possibility is seizure induction by low frequency rTMS. Although we used single pulses of TMS, we applied them approximately every 5 seconds with a small jitter of 500 ms, which could be comparable with a very low frequency stimulation of 0,2 Hz. LF-rTMS is usually supposed to reduce cortical excitability. However seizures induced by LF-rTMS in patients with epilepsy have been described [7e9]. It is possible that motor cortical plasticity may be altered in epilepsy patients, thus leading to a shift in the BCM curve which may result in LTP-like aftereffects by rTMS protocols that are supposed to induce LTD in healthy subjects [10]. The third alternative is interhemispheric disinhibition: 0,2 Hz LF-rTMS of the left hemisphere could have led to inhibition of the intact hemisphere and consecutively to inhibition of interhemispheric inhibition finally resulting in contralateral disinhibition. In that case stimulation of the affected hemisphere did not trigger seizure acitivity but LF-rTMS of the intact brain led to a slightly delayed contralateral disinhibition seizure. Eventually, a combination of all these mechanisms could have respectively contributed or rather potentiated each other.
In conclusion, although recent data suggest general safety and good tolerability of nTMS for neurosurgical preoperative mapping in a large cohort of over 700 patients [1], one should not forget that patients with cerebral lesions may still be of higher risk of seizure induction by TMS. Therefore stimulation frequency of around 0,2 Hz may still be too high in these patient population and may need to be adapted and carefully chosen, especially when mapping the contralateral intact cortex for comparison with the affected cortex.
For more information, go here.

 Read more
Read more.jpg)




